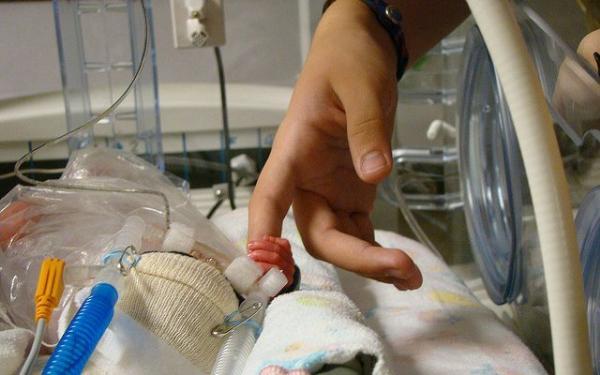
Research published recently by the British Medical Journal about the survival of severely premature babies has highlighted the difficult decisions faced by the medical professionals that care for them. Paediatric palliative care doctor, Richard Hain, presents a sensitive account of the ethical issues surrounding the provision of intensive care to premature newborns. ‘Are there children for whom intensive care and resuscitation are not appropriate?’
Last year, the BBC screened a documentary called 23 Week Babies: the Price of Life.[1] My thoughts and feelings as I watched this programme were not always straightforward. The documentary was moving, sometimes profoundly so. How could it avoid emotional impact when it dealt with life and death, compassion and vulnerability, hope and loss? There were other times when I found myself irritated and frustrated with the presenter as he made what seemed at first to be a series of ethically clumsy and unreferenced assertions.
As the programme developed, however, I realised that an editorial narrative was unfolding, and that it was one with which I could have more sympathy. There was a genuine attempt to consider the issue in a rational, as well as a compassionate, manner. Much of the presenter’s clumsiness might even, perhaps, have been carefully and deliberately provocative.
At its heart, the issue addressed by the documentary was simple enough. It was communicating to a television audience an observation already clear to those of us working in paediatrics: that we are often uncomfortable with the idea of resuscitating patients under the circumstances in which 23-week neonates are born. Though there was nothing new in the arguments themselves or their treatment, the reasons for that discomfort (the child’s own quality of life, the burden on his or her parents, issues of resource allocation) were presented in a well-scripted and thoughtful manner.
In various paediatric intensive care and palliative care forums over recent years, the broader question has been explored: ‘Are there children for whom intensive care and resuscitation are not appropriate?’ On the face of it, there is considerable unanimity in the answer among ‘intensivists’ and palliative care physicians. Most agree that there are children for whom resuscitation is inappropriate, from whom some or all intensive care interventions should be withheld.
But why? A sense of moral discomfort is surely not a robust enough base on which to build a sound ethical approach, though perhaps it is a good place to start. There is a much more important, and perhaps insidious, question that is rarely considered explicitly by clinicians: ‘What is the basis on which resuscitation of an individual child should be withheld?’ Underneath the apparent unanimity among professionals are two very different conceptions of the child that we need to consider. If we agree that some children should not be resuscitated, it still remains for us to consider the question: why?
Let me first say that I agree strongly that there are children for whom resuscitation and intensive care are not appropriate options. The interests of many of my patients are not well served by attempts at resuscitation. Withholding such measures is a manifestation of my care and concern for them as vulnerable persons. In other words, I consider that my patients should be spared it.
This stands in sharp contrast with the view represented by an intensivist with an interest in ethics who spoke at a conference two or three years ago to a mixed audience from paediatric intensive and palliative care. Like me, he felt that there were children with life-limiting conditions who should not be resuscitated. But, despite this superficial agreement, the reasons could not have been more different. The view he represented (partly, I think, in order to provoke thought) was that some children are not ‘persons’ enough to merit it. They are not, and never will be, what he considered to be fully functioning persons. It would be as reasonable, he suggested, to ventilate an intelligent monkey as a cognitively impaired child.
The argument was not, of course, laid out in quite those terms in the documentary. Nobody suggested that 23-week-old babies should demonstrate powers of rationality or self-awareness before being resuscitated. Nevertheless, the concept that they needed to ‘earn’ resuscitation was often implied. There were frequent references to the possibility that the child might be unable to develop normally. Emphasis was repeatedly laid on the fact that, of nine children who survived resuscitation at 23 weeks, only one would emerge neurologically unscathed. Irresistibly, the viewer was invited to infer that, had it been possible to identify this one at the time, he or she would properly have been resuscitated; equally irresistible was the inference that the other eight should not. The implied argument here is ambiguous. One interpretation is that survival could only be, on balance, in the baby’s best interests if the baby were normal; an argument based on the understandable (though in fact probably mistaken) assumption that there is a predictable relationship between an individual’s function and their life quality. Another interpretation, however, is that only perfectly functioning babies merit resuscitation. Seen in that way, the intuitive force of the argument is not in the effect of poor function on the baby’s life quality, but in poor function itself.
Agreement on the outcome – that children with life-limiting conditions should not always have all available resuscitation measures – therefore potentially masks a serious difference in how we consider the value of those children. On the one hand, we may consider that they deserve not to be resuscitated. On the other, we may consider that they do not deserve resuscitation. The first is an affirmation of the individual worth of every child because he or she is a person. The second is a supposition that a person’s value, and perhaps the degree to which they can be considered a person at all, varies according to their cognitive or physical function.
Children should not be resuscitated because they are not fully persons
At a recent ethics meeting, one of the participants (not a clinician), stood to say that he did not consider a newborn baby to be a sentient being. His is not an isolated view. The concept that babies (even normal ones) are not born persons, but acquire personhood somewhere after birth, is an ancient one.[2] It was indeed on this basis that in ancient times weak babies, including many of the sort of child for whom palliative medicine currently cares, would be left to die. This was not seen to be infanticide, because the baby was not yet considered to have achieved ‘personhood’.
How and when such personhood is, in fact, achieved is something that has concerned philosophers for thousands of years. The concept itself is multiply complex. It overlaps with ideas of what it is to be human, to be alive, to possess a soul, and to be made in the image of God, but it is not exactly coextensive with any of them. Personhood exists at the interface between philosophy, psychology and neurobiology, but defies attempts to reach an unambiguous definition that flows from any of them. Contemporary secular philosophers often start with the intuitive sense that to be a person requires some faculty of reason or self-awareness. Since some animals appear to possess both, this raises the possibility that some non-humans are persons.[3] Inevitably, it must also raise the possibility that some humans are not. Like the ethics meeting participant, some philosophers claim that neonates are not truly persons at all[4] and can legitimately be killed at will.[5]
So behind this is the belief that, to be a person, it is not enough simply to be a member of the species Homo sapiens; a human needs to ‘earn’ the right to be considered a person, and thus to receive those privileges reserved for persons, including, perhaps, resuscitation and intensive care.
Children deserve not to be resuscitated
One view is that children should only be resuscitated if they are likely to become fully functional. Actually, very few participants in the documentary articulated that view in isolation. More commonly, it was expressed alongside concerns that appeared to be about the child’s quality of life, directly or because of the burden on his or her parents. But although they were often expressed together, sometimes even in the course of the same sentence, these are surely fundamentally different ethical arguments. If we claim that a child’s quality of life is an important moral consideration, we have already accepted a claim that the child ‘deserves’ to be considered a person.[6]
Acceptance of that claim, which is correct, is built on a second view of moral value, namely that it is an inherent quality of being a person. During the documentary, there was the inevitable panning shot of Groningen, Holland, and I braced myself for a defence of the infamous, though perhaps misunderstood, ‘Groningen Protocol’,[7] which sets out the conditions under which a baby‘s life can be actively ended in the Netherlands. I relaxed, however, as what I actually saw was a Dutch neonatologist speaking warmly of enabling 23-week children to die in the arms of their parents, thanks to a blanket policy of withholding resuscitation at this age. Sadly, the documentary did not explore a glaring logical inconsistency at this point in its editorial narrative: if, as we had already been told, the outcome of babies of the same gestational age varies so widely, how can a blanket policy of any kind be justified ethically, even on the rather shaky moral grounds of ultimate function? Nevertheless, there was no mistaking that this neonatologist at any rate saw withholding ventilation as a kindness he was able to offer to vulnerable fellow persons. He did not withhold resuscitation because he felt there were other children with a better moral claim, or because he did not consider infants to be persons; he treated 23-week premature babies as persons who deserved something better than to be forcibly brought from the brink of a peaceful death and pierced – probably painfully – by needles and tubes.
As a paediatric palliative care doctor, this is the view that comes closest to my own. The reason I feel we should withhold resuscitation from children under some circumstances is because I consider them to be persons who deserve the treatment that will do them most good and least harm. I recognise that intensive care, for some, offers only a small likelihood of benefit to their wellbeing, while the likelihood of detriment to it is great. I am applying the same test that I would apply to introducing any medical intervention: in doing this to my patient, am I going to do more harm than good? Of course, this imposes on me the responsibility to consider a wide range of factors in many dimensions that might influence that wellbeing. As palliative care clinicians, we recognise that, for many individual patients, death is not the worst outcome; but clearly that should not mean we pre-judge the issue for any children simply on the basis of their maturity or diagnosis. These factors may or may not be relevant in individual children, but at most they are simply some of the threads that make up the skein of ethical decisions in respect of an individual. They are part of good decision-making, not alternatives to it.
So, for me, the decision to withhold resuscitation from children with life-limiting conditions is an acknowledgement that they are vulnerable children, who deserve to be protected from an inappropriate intervention. I see it as recognition of their special status as vulnerable persons, not as a claim that they have yet to earn personhood.
Ownership
A third argument seemed to emerge during the documentary. Alongside implications about the child’s need to ‘earn’ resuscitation by being neurologically normal, and compassionate acknowledgements of the child’s capacity to suffer, there were statements about the tolerability to parents of caring for such a child. The implication here seemed to be that to some extent a child can be seen to be the possession of its parents, who therefore might have the right to decide whether they can tolerate the job of caring for the child. Indeed, the Royal College of Paediatrics and Child Health (RCPCH) guidelines support withholding or withdrawal of treatment in what it describes as the ‘intolerable’ situation.[8] The question, ‘intolerable to whom?’ is not directly answered by the guidelines, though it is likely that its authors fully intended it to mean intolerable to the child. But we cannot always access the experience of the child. It is tempting instead to assess tolerability by those closest to the child whose experience we can access, namely the parents.
This is perhaps a more complex argument than it might at first appear. Parents clearly are ‘stakeholders’ in the wellbeing of their child. The capacity of parents to tolerate what is happening in respect of their child is relevant both directly because it influences them, and indirectly because it in turn influences the wellbeing of the patient, the child. The argument has been taken to a contentious conclusion by Verhagen[9] when he concluded that it was ethically acceptable for a baby with a life-limiting condition to be euthanized at the request of the child’s parents. His justification was not simply that the child was the legal possession of its parents, but that where the child cannot communicate, the interests of parents and child cannot meaningfully be separated.
Summary
It is a truism to say that at the heart of palliative care for children is the individual child. Without examining it, most practitioners working in the specialty take it as read that a child has moral value that does not have to be ‘earned’ by the capacity to move, think or even to feel. As we are increasingly having to consider issues of resuscitation and withdrawal and withholding of life-sustaining treatment, it is important to recognise that these truths are not universally acknowledged. Having answered the question, ‘Are there children for whom intensive care and resuscitation are not appropriate?’ with a reasonably unanimous, ‘Yes’, the relevant question that faces us in clinical practice is rather: ‘Is this individual child one of them ? Is intensive care with resuscitation the right intervention for this particular child?’
The ethical battle lines may seem sometimes to be drawn between those who want to resuscitate children with life-limiting conditions and those who do not. In palliative care we should not uncritically espouse either of these positions as though it were a universalisable ethical principle. We should instead insist that both resuscitation and withholding resuscitation are potentially ethically acceptable therapeutic options that should be available. Which is suitable will depend not only on the individual child and family, but on the specific circumstances under which the decision is considered. Inevitably, we will sometimes find ourselves at odds with colleagues, particularly with those from neonatal and paediatric intensive care, who may be puzzled by the inconsistency between the decisions we make in different cases.
This apparent vacillation might be read by some as a sign of uncertainty about underlying ethical principles, but in fact it is something quite different: it is the practical result of a consistent commitment to the fundamental ethical principle of compassion for individual persons.
Richard Hain is a Consultant in Paediatric Palliative Medicine and a Visiting Professor at the University of Glamorgan in Cardiff, Wales. He is a graduate student in Christian Ethics and Theology at the University of Oxford
The author would like to thank Prof John Wyatt, Dr Charles Camosy and members of the Ethics Group of Together for Short Lives for their interest in and comments on early drafts of the paper.
[1] Wishart, A., 23 Week Babies: The Price of Life, 2011.
[2] Cooper, JM., Reason and Human Good in Aristotle (Cambridge: Harvard University Press; 1975).
[3] Singer, P., Practical Ethics eBook i, iPad, editor, (New York: New York : Cambridge University Press; 2011), p. 480.
[4] Wyatt, J., '23 Week Babies - The Price of Life', Triple Helix 2011(Summer 2011):2.
[5] Verhagen, E. and Sauer, PJ., 'The Groningen protocol - euthanasia in severely ill newborns', New England Journal of Medicine, 2005;352(10):959-62, Epub 2005/03/11.
[6] RCPCH, Withholding or Withdrawing Life Sustaining Treatment in Children: A Framework for Practice, 2004 (Second Edition).
[7] Verhagen and Sauer, 'The Groningen protocol’
[8] Singer, P., 'Neonatal intensive care: How much, and who decides', Medical Journal of Australia, 1985; 142(6):335-6.
[9] Giubilini, A. and Minerva, F., 'After-birth abortion: why should the baby live?' Journal of Medical Ethics, 2012, Epub 2012/03/01.