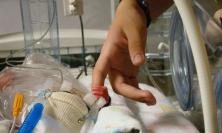
The recent death of their son Ivan drew our attention to the plight of the Cameron family and many like them who suffer the tragic bereavement of a young child. Brother Francis, a children’s palliative care nurse, describes the journey that grieving parents face, and highlights the challenges in the work of those who seek to support them.
Every child is precious and irreplaceable and the death of a child is an unbearable sorrow that no parent should ever have to endure. (Gordon Brown 2009)
Bereavement starts at diagnosis
The sad news of Ivan Cameron’s death brought to the forefront of the nation’s minds that group of parents who live with the knowledge that their child has a life–limiting or life-threatening condition. From the moment they are told that their child has such a condition these parents start to grieve; their lives are in turmoil and the whole of family life is disrupted and will never be the same again. Mr Cameron has said that discovering the scale of his son's disabilities was like ‘being hit by a freight train’. These parents have the sword of Damocles hanging over them and they just do not know when it will fall. Mr Hague said in the House of Commons:
Ivan's six years of life were not easy ones. His parents lived with the knowledge for a long time that he could die young, but this has made their loss no less heart-breaking.
The death of a child – a child who was your ‘North and your South’, a brother or sister, a much loved grandchild, or a school mate – tests our deepest beliefs. The parents who live with this pain only have a small voice, and can become isolated as their lives are taken over by caring for their child, or in some cases children. Two such parents now sit in the House of Commons, one of whom leads the country, and the other the man who would take his job; they have now been united by a tragic bond. Both have had children with a life limiting condition; both have lost a child.
What parents need throughout their journey – a journey they have little choice about taking but find themselves on nonetheless – is good pastoral care, emotional support and practical help. The challenge is to deliver this aspect of pastoral care. Having been working with families for some years now as a nurse in children’s palliative care, and with a monastic background, I have come to see that the most important aspect of the care we offer is that of presence – no easy task when we want to make the pain better, or even go away, for them.
As professionals we need to learn the art of ‘walking alongside’ the families we have the privilege of working with, and we have to learn to carry the pain and sit with the mystery of death. At some point in the journey, we must have the courage to put aside all the theories we have learnt and let ourselves be touched by the reality of the family. A bereaved parent recently wrote on a palliative care website:
Excuse me, but all of this seems to be rather a lot of unnecessarily complicated tosh. When your child is seriously ill and terminally ill, everything then depends on quality and time. The energy you have to care for your child and the professionalism and communicating qualities of the experts and carers around you... the relationships you develop are crucial, as are the sensitivities of those working with your child to you. Stress as such is not dependent on being a carer, but due to loss of control and hope. Hope comes from being there for your child in even the smallest ways...through everything, don’t rely on models, ask real people.[1]
We need to develop the skill of watching, waiting and wondering what may happen next and so need to be able to sit with silence or what Dame Cicely Saunders calls ‘silent attention’. She makes the point that those of us who have spent time in the company of people with mortal illness have learnt from them that we are always challenged to know more and to help more effectively, but above all, to listen. Sometimes there will be no answers to give to those in apparently desperate situations and we find ourselves with nothing to offer but silent attention. This is at the heart of best practice, and comes with time and experience. If we can be silent with children and parents, and refrain from asking endless questions, we will learn more about them and what they need from us.
My clinical experience informs me that the more support we can offer a family before their child dies, the less we are needed after the death. In some way it is about setting them free to do their grieving, by helping them to say the things they need to say and do the things they need to do, so they are left with very little unfinished business. When a child dies there is always ‘unfinished business’, as you will always have wanted to see them go to school for the first time, play in their first game of team sports, have their first boy or girl friend or go to university.
The aim of the work is to enable parents, siblings, grandparents, school friends to be left with what can only be described as a ‘good enough’ memory of the life, dying, death and after-care of a child, or in some cases children. It is also about leaving staff with a ‘good enough’ memory of the encounter. The Prime Minister put this well when he said: ‘I know that, in his all too brief life, Ivan brought joy to all those around him, and I know that for all the days of his life he was surrounded by his family’s love.’
Parents' responses
Rando[2] & Klass[3] state that for parents the death of a child contains dimensions not seen in other losses, including a sense of failure in their parental role as ‘protector’.
To live through the death of your child is perhaps one of the most painful experiences known to humankind. It is instinctive in parents to nourish and protect their child. Death is to be fought, even to the point of sacrificing your own life, but sometimes the fight is lost. Life is literally beyond control. The death of your child leaves you feeling helpless, guilty, powerless and broken.[4]
Parents also suffer a sense of loss of self, because of the investment of their hopes for the future in their children. Grief for parents has no fixed end nor can a pre-grief state ever be regained. This has clear implications for the type of pastoral care bereaved parents are offered, and for when and how it is offered to them. The deeply stressful event can leave a parent with mental health issues, which will hinder their long-term adjustment and lead to what is sometimes called ‘complicated grief’. As part of this they may lose their faith or trust in God and the Church. How we care for them before their child dies is a key factor in their long-term survival and their adjustment to life without their child.[5]
Before death, and at the time of death, parents need to maintain some sense of control. Moulton[6] found that parents who felt at least partly in control were able to find some ‘peace and serenity’; conversely, those that had no control felt guilty. My experience suggests it is crucial to make parents aware of what choices are available to them, so they can plan for the death of their child in their place of choice.
Nothing can turn the clock back: no text can mend the torn hearts of parents whose child has died, but how we work with them can either help them or block them on their journey. Surkan et al write that families who report that their child’s care was sub-optimal spoke of more frequent feelings of guilt in their bereavement, compared to families who felt their child and they were well cared for.
Rolls & Payne[7] found that parents struggled to maintain their parenting role as they coped with their own bereavement and the disruption of their circumstances, which can add to their feelings of guilt. Craft & Killen[8] found in their independent review of services that parents were asking for more bereavement support for siblings. For me, in my clinical work, it is the siblings that are the most important as they can be forgotten and can feel both very guilty and angry at the same time.
My attempts to prepare Andrew’s sisters were totally insufficient. It should have started earlier and with professional help. The prospect of my own loss was so great I could not sufficiently appreciate my daughters’ loss.[9]
One thing I have learnt over the years is that it seems parents of dying children are all on similar journeys and face similar issues. I have not met a parent in this situation who has not known at a deep level that their child is dying; however, what they present to the outside world may be seen as denial. In fact, what they are doing is coping or ‘getting through the day in one piece’; it is called ‘maintaining their hope’. If we misread this, we may well intervene in the wrong way. They need their hope as this gets them through the day and helps them hold things together for the rest of the family, and they need us to support them in this. This is not some form of collusion; it is understanding how they cope and what they need at that time. If we fail to understand how a family works, what roles they have and how they process information, we may well miss a trick and intervene in the wrong way, or in a way that can be unhelpful and subsequently affect our relationship with the parents, which in turn will affect the care given to the child or sibling.
This point was illustrated to me a few years ago when a well-meaning medical consultant and a community nurse felt a mother did not fully understand how ill her child was and they saw it as their job to tell her. They took the mother into a side room late one Friday afternoon, and told her that her child was very ill and could die very soon, maybe even over that weekend. The mother left the room very angry with the two professionals and took her child home. Planning meetings after this event had to take place in a GP’s office, as the mother would not return to the hospital. These professionals did not fully understand how the mother and child talked with each other, nor how the mother liked to transmit messages to her child. I would suggest that their intervention was more about their needs than those of the child and mother.
I have come to see over the years that suffering is not a question that demands an answer, it is not a problem that demands a solution; it is a mystery that demands a presence. This seems countercultural in a strange way, as we are all trained to ‘make things better’ and to be always doing something. It can be painful for care staff to see a child die and a family grieve, but it is important that we acknowledge this fact so that we can care for each other and ourselves as we do this work, as well as doing what is best for the family – sometimes this might mean taking a step back and rethinking what we assume is for the best, which can be very difficult.
Strategies for meaningful and helpful intervention
The key for me in my clinical work is this: what do we mean by meaningful and helpful interventions, what can we do as health care professionals? The answer is both clear and complicated. In reality there is very little we can do that will make this situation better. However, I think there is a great deal we can do to help children and parents during this time. Sir Luke Fildes’ painting, ‘The Doctor’ (which can be seen here), is an eloquent portrayal of what our work is all about: the doctor is attending the child, watching, waiting and wondering, ‘being there’. He is there, which is by far the most important thing he, or we, can do. Most of the painting’s impact is in the space between the physician’s eyes and the child, which is filled, solely, by the doctor’s gaze, full of humanity. As always with children, it is set in the context of the grieving family, who you can just see in the background. I think I am right in saying that this family had lost two other children, and it is worth noting that the painter had also lost his own child. We must never forget the family in the background of any story; we do so at our peril.
An attending practitioner is someone who is present to the moment, believing that this moment is the moment. To wait with openness and trust is an enormously radical attitude towards life and our work, and more so in these times of great stress on the family and staff. It beckons us to become good listeners and not necessarily doers. Listening is not just about hearing: hearing refers just to sounds, listeningrequires focusing on the whole patient. It means paying attention not only to the story, but to how it is told, to the use of language, both voice and body. For me it is more about listening for what is not being said, for the gaps in the story.
Palliative care is about being present to the child. Children need us to be present and not bring presents, which is what they normally get when they are dying or their sibling is dying. But what they need most of all is for us to give them our full attention so they can do the work they need to do before they move on to the next stage of their journey. The same can be said for the family.
How can I evidence this statement, you may well ask? Well, I can’t. Evidence is hard to come by in this area, but we do have clinical experience from which we can draw some conclusions and some guidance on how to work with parents who are grieving and who will lose their child.
Creating a sacred space
On this journey, we need to learn to sit, to watch, to wait and let ourselves wonder. We need to recognise that the most we can do is to prepare and hold the space where the miraculous may happen. It is in the creating of this compassionate space that all things may arise: sorrow, loneliness, desire, regret, frustration, and happiness.
We have to create a safe and secure space, or what I would call a sacred space, where the child or family can express their inner suffering and know that it is all right to do so, that they will be heard and taken seriously. A sacred space is unique and will mean different things to different people. The uniqueness comes from the meaning and the value that the individual allots to that sacred space. It is a place of safety – emotional and physical. It is a place a family can go, emotionally or physically, to get some dedicated time exclusively for them; a space away from all the trauma that may be going on in their world. It is a space where a sense of self can be restored, where they can make sense of this new and painful experience, and they can refresh their energy.
When life feels blurred or confused we need this sacred space to focus on ourselves and restore perspective. If a parent or child is supported to spend time in their sacred space, it makes them more available for what may be happening at home or in hospital.
Preparing and holding the space is what we do when we offer ‘expert’ and effective pastoral care; we create a warm and friendly environment for the families we work with, and we can help open up blocked channels of communication as we work with distressed families who can find no meaning in their child’s illness, suffering or death, and who struggle to make sense of the puzzle of life.
If we can find a creative way of responding to the challenge of grief, it may open up a path to the very heart of living, even in the shadow of death.
Brother Francis, OSB, RGN, RSCN, B. Sc (Hons) is a Nurse Consultant in Children’s & Young People's Palliative Care in the North of Scotland.
[2] Rando, T. A. (1986), ‘Parental Bereavement: An Exception to the General Conceptualisations of Mourning’ in Rando, T. A. (Ed.) Parental Loss of a Child, Illinois, Research Press.
[3]Klass, D (1996), ‘The deceased child in the psychic and social worlds of bereaved parents during the resolution of grief’, in D. Klass, P. Silverman & S. Nickman (eds), Continuing bonds: New understanding of grief, Taylor & Francis, Washington, DC, pp. 199-215
[4] Dominica, F (1997), Just My Reflection, DLT, UK
[5] See Surkan, P., Kreicbergs, U., Valdimarsdottir, U., Nyberg, U., Onelov, E. & Dickman, P. (2006), ‘Perceptions of Inadequate Health Care and Feelings of Guilt in Parents after the Death of a Child to a Malignancy: A Population-Based Long-Term Follow-Up’, Journal Of Palliative Medicine, Volume 9, Number 2, 2006 and Riley, L., LaMontagne, L., Hepworth, J., Murphy, B. (2007), ‘Parental Grief Responses And Personal Growth Following The Death Of A Child’, Death Studies, 31, pp. 277–299, 2007
[6] Moulton, M. (1997), ‘Maternal Responses to the Life and Death of a Child with a Developmental Disability: a story of Hope’, Death Studies 21, Vol 5, pp. 443 - 476
[7] Rolls & Payne (2007), ‘Children & young people’s experience of UK childhood bereavement services’, Mortality, Vol 12, No. 3, pp. 281 – 303.
[8] Craft, A. & Killen, S. (2007) Palliative Care Services for Children and Young People in England: An independent review for the Secretary of State for Health, DOH Publications
[9] Darnill & Gamage (2006), ‘The patient’s journey: palliative care – a parent’s view’, BMJ, Vol 332, pp. 1494 - 1495